When it comes to writing a birth plan, most of us focus on things like pain relief strategies and playlists, but one Sydney obstetrician says there is a single line that should always be in bold.
Professor Peter Dietz from the University of Sydney has dedicated his research career to understanding pelvic floor trauma from childbirth, and has come to the conclusion that forceps should be avoided unless absolutely necessary for a mother and baby’s safety.
“The one thing that any woman can do to avoid [pelvic floor trauma] is to avoid forceps,” he tells Kidspot.
Professor Dietz points to research showing women who have a forceps delivery are 10 times more likely to have a future prolapse than women who have had a caesarean and are twice as likely to have one compared to women who had a vacuum delivery. Using forceps also doubles a mother’s risk of anal sphincter tears compared to vacuum and doubles the risk of anal incontinence compared to other delivery modes.
It’s enough to make any pregnant woman curl up in an anxious ball but Professor Dietz says that if you make clear in your birth plan that you do not want forceps used unless it’s a matter of life and death, then there is a very good chance that the medical team will honour your wishes and still get your baby out safely.

Babies can be born safely without forceps in most situations. Image: Unsplash.
Express preferences but don’t be absolute
“Write a birth plan with your preferences – I would say, ‘Under no circumstances do I agree to a forceps delivery unless the baby is in immediate danger and cannot be delivered in any other way’,” he suggests.
“Don’t be too absolute because you do have to go with the flow, but you can express preferences.”
Professor Dietz believes that in cases where a baby needs assistance getting out, a vacuum or even a caesarean, is much safer for the pelvic floor.
In fact, he says the Swedish College of Obstetrics and Gynaecology has recommended forceps no longer be used, and he says they haven’t been used in Denmark for 15 years, which he says has reportedly led to better pelvic floor outcomes for mothers.
“In Australia, we should be way ahead of anywhere else in the world and the opposite is the case,” he says.
“As many as 12 percent of births occur with forceps in some Australian hospitals [but] obstetrics can be done without forceps.”
By having it written clearly in your birth plan, Professor Dietz says you should be able to avoid having to worry about expressing your no forceps wishes in the heat of the moment.
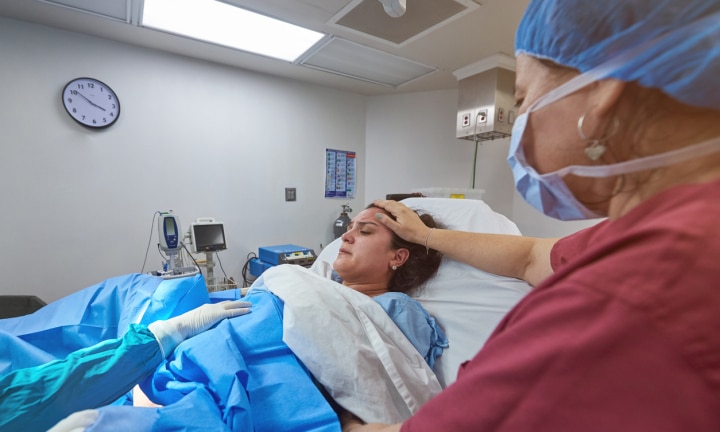
Don’t leave it till the heat of the moment. Image: iStock.
It’s worth noting that some obstetricians express concern that caesareans can present risks to future pregnancies and children’s ongoing health.
“Obstetricians are aware of the various risks of caesarean versus vaginal delivery and should help to guide the patient in making a decision,” Stefan Hansson, professor in obstetrics and gynaecology at Lund University, writes on The Conversation.
“Patients should be informed of all of the risks – at all life stages, for mother and child – and assess their options based on that.”
Other things you can do to protect your pelvic floor
While some experts suggest that birthing in a squatting position and trying not to push too hard or early can be protective for the pelvic floor muscles, Professor Dietz believes that’s not always sensible, given it can make it more difficult for midwives to support the perineum while you deliver.

Birthing in a squatting position can be dangerous. Image: istock.
“It’s much harder for a midwife to have a hand there to slow things down when the baby’s head crowns,” he says.
“The more people are upright, the more the tissues become waterlogged due to reduced lymphatic drainage, which makes tears more likely.”
Professor Dietz says that an epidural is not a bad idea for pelvic floor protection either.
“An epidural may have some advantages for the pelvic floor because it relaxes the tissues down there,” he says.
Meanwhile, keeping up the Kegels during pregnancy is wise for helping the muscles bounce back post-childbirth.
“Pelvic floor exercises certainly don’t hurt – it’s good policy to work that muscle,” he says.
“But it doesn’t look as if you can prevent damage by doing them – the best thing you can do in that regard is have a birth without forceps.”
Don’t stress too much about pelvic floor damage
If you’ve had a pelvic floor injury after one birth, you might understandably be nervous about subsequent births, however Professor Dietz says it’s important to note that few women are injured in later births.

Major pelvic floor injuries occur in a minority. Image: istock.
“Second babies don’t seem to do more damage to the pelvic floor,” he says.
And for first-time mothers, he says it’s good to know that major pelvic floor injuries occur in a minority, and that if forceps aren’t used then your chances of pelvic floor injury are actually small.
“In most instances everything is fine,” he says.
“When it comes to the pelvic floor, for over half of women who have vaginal births, things look just the same afterwards.”
This article was first published on Kidspot.
ALSO READ: Mummies, Here Are 5 Things That Will Utterly Ruin Your Birth Plan
 Together Against RSV
Together Against RSV Pregnancy
Pregnancy Parenting
Parenting Child
Child Feeding & Nutrition
Feeding & Nutrition Education
Education Lifestyle
Lifestyle Events
Events Holiday Hub
Holiday Hub Aptamil
Aptamil TAP Recommends
TAP Recommends Shopping
Shopping Press Releases
Press Releases Project Sidekicks
Project Sidekicks Community
Community Advertise With Us
Advertise With Us Contact Us
Contact Us VIP
VIP Rewards
Rewards VIP Parents
VIP Parents
